|
||||
| The Angio Institute | Research & Education | Brain Health Program | AngioNews/Media | Joining Hands |
MEET THE BRAIN HEALTH PROFESSIONAL ALLIANCE
IPHA- The Integrative Pain Healers Alliance (with support from the AngioFoundation outreach initiative) has forged an educational partnership of independent clinical experts, pioneers, caregivers and advocates. This year, IPHA is proud to unite academic leaders to build the BRAIN HEALTH COLLECTIVE. This set of contributors are joined to expand current research in cognitive issues, cerebral wellness and the vast set of studies about the mind-body connection. The IPHA BRAIN HEALTH COLLECTIVE will publish educational topics about current studies on advanced innovations and protocols in support of functional health sciences. Meet the crusaders in the field of Cognitive Health covering a wide spectrum of studies and initiatives from neuroscience, mental health/psychotherapy, concussion treatments, brain cancer research, sports injury studies, biotech engineering and diagnostic sciences. In addition, our team also includes advocates and survivor coaches with first-hand experience in TBI or Brain Injuries. This unique panel of professionals presents their expertise and offers their insight on the current state of health & wellness from their respective work - while collaborating with each other in the name of research or public education. [Photos TBA] |
||||||||
Clinical Research Program
One in 11 people in USA will be diagnosed with PTSD in their lifetime (according to the APA), whereas women are twice as likely as men to have PTSD. A clinical study led by Dr. Paul Dreschnack is to be launched by mid-2023 based on the application of regenerative integrative medicine where PTSD patients will be treated following the study protocol which is currently in progress of submission to The Institute of Regenerative and Cellular Medicine Independent Review Board for the FDA. Patients shall be closely monitored by a team of diagnostic specialists monitoring treatment response through advanced quantitative imaging and metabolic/epigenetic testing. Under collaboration with board certified psychiatrists, data gathering and observational reporting, our team's objective aims to address the triggers of PTSD and hopes to arrest the sequence of events that cause such a high suicide rate among our veterans.
|
||||||||
| Educational Programming | ||||||||
|
|
|
||||||
2022 Presentation: Healing After Covid-19: Impacts in Pediatric Medulloblastoma
By: NOELLE CUTTER, Ph.D, Assoc. Professor of Biology & Chemistry - Molloy University / NY Cancer Resource Alliance
In collaboration with NYCRA scientific panel experts: ROBERT BARD, MD and ROBERTA KLINE, MD
 |
 |
 |
This video presentation is part 2 of Dr. Noelle Cutter's 2021 presentation on the Impact of Covid-19 in Pediatric Medulloblastoma. It includes a collaboration with Dr. Robert Bard (cancer imaging specialist) and Dr. Roberta Kline (leading genomics advisor). Medulloblastoma (MB) is a devastating illness and is the most common pediatric malignant brain tumor. It is predominantly treated with cytotoxic and nontargeted approaches. Survivors of MB also suffer from severe treatment-related effects of radiation and chemotherapy keeping mortality rate high.
Over the last several years, remarkable technological breakthroughs have facilitated the molecular characterization of multiple tumor types, provided new insights into the genetic basis of these cancers, and prompted innovative strategies that are changing the management paradigm in pediatric neuro-oncology. Genomic tests have begun to affect medical decision making in several ways, from delineating histopathologically similar tumor types into distinct molecular subgroups that correlate with clinical characteristics, to guiding the addition of novel therapeutic agents for patients with high-risk or poor-prognosis tumors, or alternatively, reducing treatment intensity for those with a favorable prognosis. However, the impact of COVID19 may have on the pediatric population, and the management of children with cancer, remains unclear and poorly documented. (See complete video)
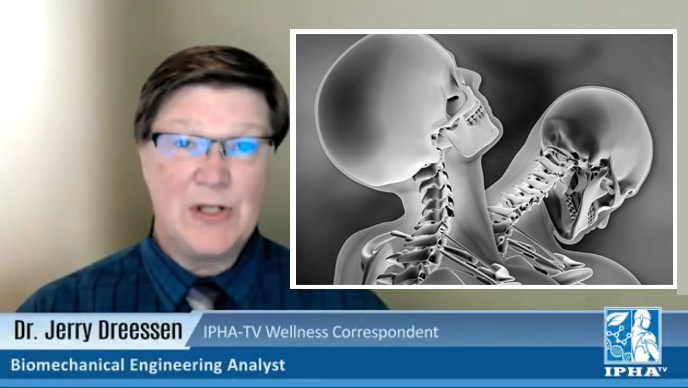
OPTICSCAN: NEURO-TESTING FOR CONCUSSION METRICS
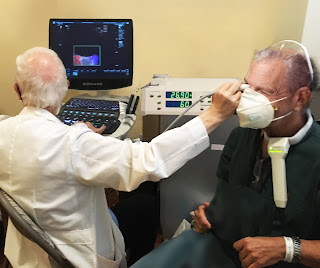
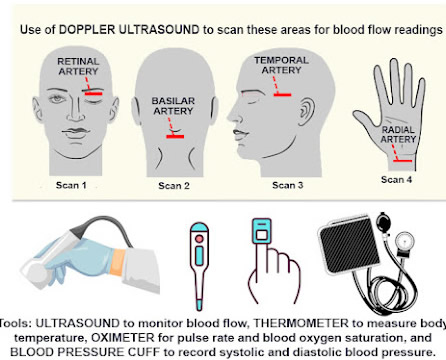
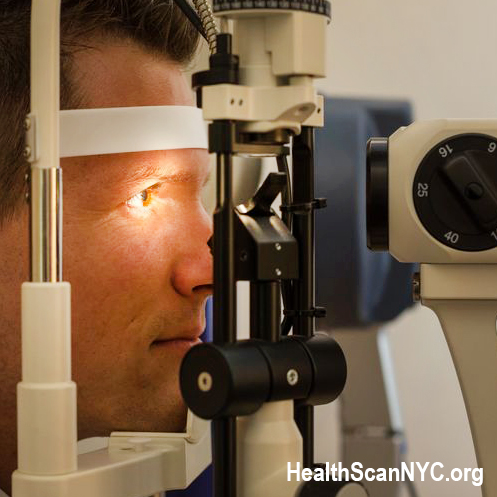
A new study is underway at THE BARD CANCER CENTER IN NYC. Dr. Robert Bard and a local research team combines the latest biometric scanning advantages of transcranial DOPPLER imaging, hemodynamic ULTRASOUND scanning (of the retinal, basilary and temporal arteries) and the integration of BIOFEEDBACK technology for a special research study. This neuro-scan review establishes (1) a cross-comparative study between the technologies and (2) a multi-modality screening & monitoring protocol to record post-concussion and neurodegenerative disorders. THEORIES AND OBJECTIVES: Neuroscanning aims to identify any/all biometrics recorded through the use of standard and approved medical imaging technologies (like 3D Doppler Ultrasound). Use of noninvasive diagnostic tools used in this study are selected based on their anticipated ability to collect baseline data. It is also often used as comparative assessment of any therapeutics or response from outside stimulation. SELECTED AREAS SCANNED WITH ULTRASOUND: Autoregulation of the circulatory system is controlled by several homeostatic mechanisms including the autonomic nervous system, which is believed to be a mechanism by which meditation alters cardiovascular function. As such, evaluating blood vessel flow and function aligns with studying the body’s effects under a meditative state. According to Dr. Robert Bard, the areas of the body scanned with ultrasound are key areas that have the highest probability of response and reaction from a device that claims to promote bringing the subject into a meditative state. The chosen target scan areas (Basilar Artery, Eye/Optic Nerve, Temporal Artery and Radial Artery) are identified as key zones for hemodynamic study, showing the most effective areas for studying blood flow. |
|||
Research Review: Neurodegenerative Diseases and the Vascular System
The notion that neurological diseases are preventable will evolve over time, as has already been seen in with a greater understanding of cardiovascular disease. The field of cardiology has become much more proactive in addressing cardiovascular health, where identifiable and modifiable risk factors can be assessed by clinicians and used to prevent or address heart and vascular disease earlier on in the process. This is directly applicable to neurological diseases, as there is a growing recognition that vascular factors play a critical role in brain health. Now that radiologists are using Doppler blood flow to examine eye disease, including systemic diseases (including Diabetes, Brain tumors, heart disease, sickle cell disease etc) that affect the eye, we are hopeful that the ophthalmologic and neurological communities will start using this noninvasive technology as well to improve noninvasive and more rapid treatment of potential eye disorders, such as cancers of the eye, diabetes and glaucoma. Another future use will be to correlate the effect of decreased vascular pulsation in the production of cerebrospinal fluid that is removed by the cleansing glymphatic system is postulated as a contributing factor in degenerative neuromuscular disease. |
|||
Global Research Alliance Targeting the MENTAL HEALTH CRISIS The Coronavirus Pandemic scorched the global community with unprecedented health effects on its countless victims (from cardiopulmonary issues to neurological damage etc). Mitigating the rise in infection and mortality rates called for a 'borderless' collective of scientists and medical experts to form a mass research initiative. This joint effort brought us the worldwide vaccine development, prevention & prophylactic solutions, geo-social intervention and diagnostic innovations. This includes post-infection disorders (long haul) are the next major concern, demanding quantifiable research and treatment protocols.
From economic stresses to social isolation to fears of infection from a deadly virus, SARS-CoV-2 has also driven an unprecedented MENTAL HEALTH crisis. Since mid-2020, national news and mental health professionals reported an unusually high rate of substance abuse, depression, suicide cases and a major spike in public violent (anger and rage-driven) crimes [1] [2] [3]. In March of 2021, the AngioFoundation formed an integrative coalition of mental health and clinical experts to review the top innovations and modalities to focus on this pandemic related list of mental health issues. "The strategy behind the use of multiple protocols to battle any health issue or crisis has always been the most effective solution (historically) in medical care," states Dr. Robert Bard, cancer diagnostic expert. "Decades in cancer care has proven that there is NO ONE ANSWER TO CANCER... meanwhile, having multiple sets of options within integrative medicine helps to provide the best chance of success. We apply this concept towards depression, PTSD or even suicidal tendencies... we are now seeing breakthroughs in areas like medical imaging to track and quantify physiological and neurological evidence aligned with these disorders. These innovations can only add a new level of detection, data measurement and tracking confirmation to support patient care professionals, and aid in the treatment (and reversal) of our global mental health crisis."
|
|||
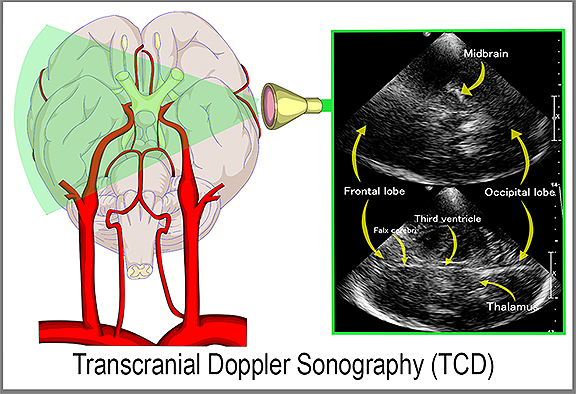
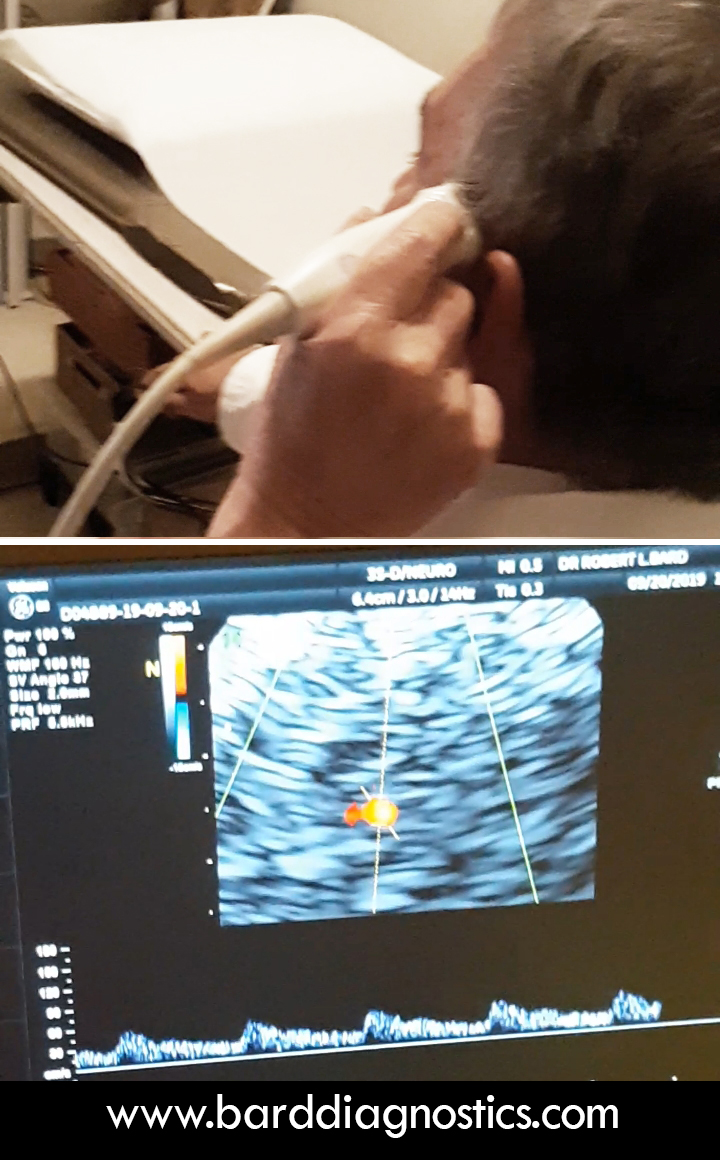
Cranial Scan & Neuro-Imaging of PTSD Emotional traumas and stress influencers are scientifically aligned with anxiety, depression, behavioral disorders, drug/alcohol abuse and a wide list of physiological health issues. These symptoms are typically diagnosed by mental health professionals through observational science and behavioral analysis. But within the past 15 years, global advancements in transcranial imaging pioneered the ability to detect trauma-related issues in the brain through neurological imaging. Now, neurological stress can be identified clinically by monitoring chronic imbalance and changes in the neurochemical structure (or circuitry). The shift in memory performance - specifically the hippocampus and the medial prefrontal cortex is one indicator of this imbalance whereby a stressful event can show images with signs of neuronal dysfunction. Neuro-imaging measures brain thought activity which has known chemical tissue changes by observing the alterations in capillary blood vessels in the retina located in close proximity to the main emotional center of the anterior brain. Functional MRI (fMRI)* is currently used to show brain chemical changes with cognitive commands such as “death vs freedom.” Most recognizable patterns with suicide occur in the anterior cingulate cortex of the brain which lies directly behind the globe and is vascularized by orbital branches of the anterior cerebral artery. Functional near infrared imaging (fNIR) devices show changes in brain oxygenation linked to suicide. Another imaging innovation is the TRANSCRANIAL DOPPLER (TCD) - a type of sonogram that is a non‐invasive, non‐ionizing, inexpensive, portable and safe technique that uses a pulsed Doppler transducer for assessment of the blood flow in the anterior cerebral arterial circulation. This technology has been used to evaluate intracranial steno‐occlusive disease, subarachnoid hemorrhage, and extracranial diseases (including carotid artery disease and subclavian steal syndrome), detection of microembolic signals and acute strokes. The Transcranial Doppler has been used to examine the mean speed of blood circulation of patients to validate and monitor treatment efficacy by tracking cranial blood vessels and vertebrobasilar flow vasospasm. *See Video: PTSD Research Through fMRI -by Dr. Ruth Lanius <YouTube Link> Video by London Free Press, a division of Postmedia Network Inc. |
|||
Psychoanalysis and Optical Brain Imaging in vivo
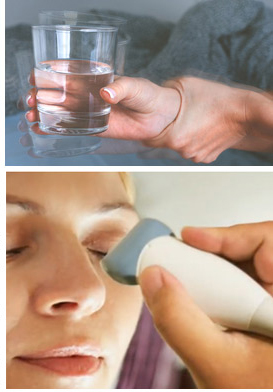
Another device used by imaging specialists to detect mental distress is through an EYE SONOGRAM or Real Time Sonofluoroscopy of the orbital soft tissues of the eyes. This process is performed in multiple scan planes with varying transducer configurations and frequencies. Power and color Doppler use angle 0 degrees and PRF at 0.9 at the optic nerve head. 3D imaging of optic nerve and carotid, central retinal arteries and superficial posterior ciliary arteries performed in erect position before & after verbal communication and orbital muscle tissue contractions may be observed as a precursor to visual changes in facial expression. Retinal arterial directional flow is also measured with peak systolic and diastolic values. Bulging of the optic nerve head is checked as increased intracranial pressure may be demonstrable in this condition. Other innovations such as the TRANSORBITAL DOPPLER, 3D/4D VESSEL DENSITY HISTOGRAM and the RETINAL OCT (optical coherence tomography) are also being explored in the pursuit of studying brain performance through the eyes. An expanded review on these solutions will be available in part 2 of this report. Suicide and PTSD
Considerable research has reported a strong connection between significant forms of trauma and suicides or similar behaviors. Moreover, additional claims indicate an elevated number of cases from individuals with mental illness. With military Veterans, for example, combat-related traumas have been closely monitored to indicate a heavy preoccupation to self-inflict injury as a means of engaging recurrent nightmares, relenting negativity, high emotions of high anxiety, anger or guilt acquired from times of active duty. These cases are often scalated by clinical depression, substance abuse and suppressed or hidden emotions that result in uncontrollable reactions. [1] Suicide rates have been rising in nearly every state, according to the latest Vital Signs report by the Centers for Disease Control and Prevention (CDC). In 2016, nearly 45,000 Americans age 10 or older died by suicide. Suicide is the 10th leading cause of death and is one of just three leading causes that are on the rise. [2]. Approximately 23% of people who had experienced a physical assault had also attempted suicide at some point in their life. These rates of suicide attempts increased considerably among people who had experienced multiple incidents of sexual (42.9%) or physical assault (73.5%). [3] Further, some cognitive styles of coping such as using suppression to deal with stress may be additionally predictive of suicide risk in individuals with PTSD. [4] 1) The Major Occupational Hazard of Post Traumatic Recall - Journal of Modern Healing Occupational Hazard of Post Traumatic Recall
High risk professions like law enforcement, military service, healthcare and emergency response are known to have exposure to some of the most extreme levels of trauma - both physically and psychologically. They range in effects from manageable symptoms to crippling disorders. Over time, most people overcome disturbing or traumatic experiences and continue to work and live their lives. But others who get affected by traumatic experiences may trigger a reaction that can last for months or even years. This is called Post-traumatic Stress Disorder, or PTSD. Proportionately, studies have shown a lower percentage of retirees from such challenging careers acquire PTSD (from 15-20%) while an estimated 30-40% who suffer from PTSD associated symptoms go undetected or do not register as full cases. A larger percentage ‘on the job’ might be able to maintain the expected work standards throughout their career and even make it to retirement without visible signs. But “POST traumatic recall” leading to fully blown PTSD occurs when repeated exposure to trauma compounds on the tolerance capacity that eventually, one’s coping ability collapses. The individual may feel stages of grief, depression, anxiety, guilt or anger from uncontrollable issues like recurring flashbacks and nightmares. Enduring trauma is different and unique for everyone. Some cases are event-specific (having intense auditory impact or visual intensity of a terrifying event) while other cases are contingent upon the tolerance of an individual. There are people who are more emotionally expressive than others- and that might help with if they talk about the trauma that they've been through. A latent emotional disorder like PTSD symptoms can come out over time just like anything that is suppressed or repressed. It could take some time for somebody who came back from combat or a first responder who has been in a traumatic event to show signs of disturbance. They could be holding it in and repeatedly thinking about it privately (or ruminating over it) allowing the disturbing memories to get more intense by the day. This can often be a coping mechanism- protecting themselves from dark or negative feelings for a while, but eventually it builds up and can become symptomatic like flashbacks and anxiety, then leading to an eventual explosion. Meanwhile, some people just have flashbacks right after the experience because of the way that everybody's brain processes differently. Others obsess over thoughts that keep popping up over and over again. It really just depends on the person.
Disclaimer & Copyright Notice: The materials provided on this website are copyrighted and are the intellectual property solely of the publishers/producers (The AngioFoundation / the NY Cancer Resource Alliance / IntermediaWorx inc). It is provided to you solely for your own personal, non-commercial use and not for purposes of resale, distribution, public display or performance, or any other uses by you in any form or manner whatsoever. Unless otherwise indicated on this Internet web site, you may display, download, archive, and print a single copy of any information on this Internet web site, or otherwise distributed from us for such personal, non-commercial use. Also, certain content may be licensed from third-parties. The licenses for some of this Content may contain additional terms. When such Content licenses contain additional terms, we will make these terms available to you on those pages, in the Terms of Use or in the Additional Information section of our Site (which his incorporated herein by reference).The publishers/producers of this website and the contents of this website such as videos, graphics, text, and other materials published are for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. For any questions you may have regarding a medical condition, please always seek the advice of your physician or a qualified health provider. Do not postpone or disregard any professional medical advice over something you may have seen or read on this website. If you think you may have a medical emergency, call your doctor or 911 immediately. This website does not support, endorse or recommend any specific products, tests, physicians, procedures, treatment opinions or other information that may be mentioned on this site. Referencing any content or information seen or published in this website or shared by other visitors of this website is solely at your own risk. The publishers/producers of this Internet web site reserves the right, at its sole discretion, to modify, disable access to, or discontinue, temporarily or permanently, all or any part of this Internet web site or any information contained thereon without liability or notice to you.
|